User:Mr. Ibrahem/Tuberculosis
| Tuberculosis | |
|---|---|
| Other names | Phthisis, phthisis pulmonalis, consumption |
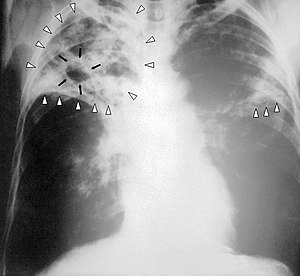 | |
| Chest X-ray of a person with advanced tuberculosis: Infection in both lungs is marked by white arrow-heads, and the formation of a cavity is marked by black arrows. | |
| Medical specialty | Infectious disease, pulmonology |
| Symptoms | Chronic cough, fever, cough with bloody mucus, weight loss[1] |
| Causes | Mycobacterium tuberculosis[1] |
| Risk factors | Smoking, HIV/AIDS[1] |
| Diagnostic method | CXR, culture, tuberculin skin test[1] |
| Differential diagnosis | Pneumonia, histoplasmosis, sarcoidosis, coccidioidomycosis[2] |
| Prevention | Screening those at high risk, treatment of those infected, vaccination with bacillus Calmette-Guérin (BCG)[3][4][5] |
| Treatment | Antibiotics[1] |
| Frequency | 25% of people (latent TB)[6] |
| Deaths | 1.5 million (2018)[7] |
Tuberculosis (TB) is an infectious disease usually caused by Mycobacterium tuberculosis (MTB) bacteria.[1] Tuberculosis generally affects the lungs, but can also affect other parts of the body.[1] Most infections show no symptoms, in which case it is known as latent tuberculosis.[1] About 10% of latent infections progress to active disease which, if left untreated, kills about half of those affected.[1] The classic symptoms of active TB are a chronic cough with blood-containing mucus, fever, night sweats, and weight loss.[1] It was historically called "consumption" due to the weight loss.[8] Infection of other organs can cause a wide range of symptoms.[9]
Tuberculosis is spread from one person to the next through the air when people who have active TB in their lungs cough, spit, speak, or sneeze.[1][10] People with latent TB do not spread the disease.[1] Active infection occurs more often in people with HIV/AIDS and in those who smoke.[1] Diagnosis of active TB is based on chest X-rays, as well as microscopic examination and culture of body fluids.[11] Diagnosis of latent TB relies on the tuberculin skin test (TST) or blood tests.[11]
Prevention of TB involves screening those at high risk, early detection and treatment of cases, and vaccination with the bacillus Calmette-Guérin (BCG) vaccine.[3][4][5] Those at high risk include household, workplace, and social contacts of people with active TB.[4] Treatment requires the use of multiple antibiotics over a long period of time.[1] Antibiotic resistance is a growing problem with increasing rates of multiple drug-resistant tuberculosis (MDR-TB) and extensively drug-resistant tuberculosis (XDR-TB).[1]
As of 2018 one quarter of the world's population is thought to have latent infection with TB.[6] New infections occur in about 1% of the population each year.[12] In 2018, there were more than 10 million cases of active TB which resulted in 1.5 million deaths.[7] This makes it the number one cause of death from an infectious disease.[13] As of 2018, most TB cases occurred in the regions of South-East Asia (44%), Africa (24%) and the Western Pacific (18%), with more than 50% of cases being diagnosed in eight countries: India (27%), China (9%), Indonesia (8%), the Philippines (6%), Pakistan (6%), Nigeria (4%) and Bangladesh (4%).[13] The number of new cases each year has decreased since 2000.[1] About 80% of people in many Asian and African countries test positive while 5–10% of people in the United States population test positive by the tuberculin test.[14] Tuberculosis has been present in humans since ancient times.[15]
References
[change | change source]- ↑ 1.00 1.01 1.02 1.03 1.04 1.05 1.06 1.07 1.08 1.09 1.10 1.11 1.12 1.13 1.14 1.15 "Tuberculosis (TB)". www.who.int. Archived from the original on 30 July 2020. Retrieved 2020-05-08.
- ↑ Ferri, Fred F. (2010). Ferri's differential diagnosis : a practical guide to the differential diagnosis of symptoms, signs, and clinical disorders (2nd ed.). Philadelphia, PA: Elsevier/Mosby. p. Chapter T. ISBN 978-0-323-07699-9.
- ↑ 3.0 3.1 Hawn TR, Day TA, Scriba TJ, Hatherill M, Hanekom WA, Evans TG, et al. (December 2014). "Tuberculosis vaccines and prevention of infection". Microbiology and Molecular Biology Reviews. 78 (4): 650–71. doi:10.1128/MMBR.00021-14. PMC 4248657. PMID 25428938.
- ↑ 4.0 4.1 4.2 Organization, World Health (2008). Implementing the WHO Stop TB Strategy: a handbook for national TB control programmes. Geneva: World Health Organization (WHO). p. 179. ISBN 978-92-4-154667-6. Archived from the original on 2 June 2021. Retrieved 28 July 2020.
- ↑ 5.0 5.1 Harris, Randall E. (2013). Epidemiology of chronic disease: global perspectives. Burlington, MA: Jones & Bartlett Learning. p. 682. ISBN 978-0-7637-8047-0.
{{cite book}}: External link in|ref= - ↑ 6.0 6.1 "Tuberculosis (TB)". World Health Organization (WHO). 16 February 2018. Archived from the original on 19 September 2018. Retrieved 15 September 2018.
- ↑ 7.0 7.1 "Global Tuberculosis Report" (PDF). WHO. WHO. 2019. Archived (PDF) from the original on 17 December 2019. Retrieved 24 March 2020.
- ↑ The Chambers Dictionary. New Delhi: Allied Chambers India Ltd. 1998. p. 352. ISBN 978-81-86062-25-8. Archived from the original on 6 September 2015.
- ↑ Adkinson, N Franklin; Bennett, John E; Douglas, Robert Gordon; Mandell, Gerald L (2010). Mandell, Douglas, and Bennett's principles and practice of infectious diseases (7th ed.). Philadelphia, PA: Churchill Livingstone/Elsevier. p. Chapter 250. ISBN 978-0-443-06839-3.
- ↑ "Basic TB Facts". Centers for Disease Control and Prevention (CDC). 13 March 2012. Archived from the original on 6 February 2016. Retrieved 11 February 2016.
- ↑ 11.0 11.1 Konstantinos A (2010). "Testing for tuberculosis". Australian Prescriber. 33 (1): 12–18. doi:10.18773/austprescr.2010.005.
- ↑ "Tuberculosis". World Health Organization (WHO). 2002. Archived from the original on 17 June 2013.
- ↑ 13.0 13.1 "Global tuberculosis report". World Health Organization (WHO). Archived from the original on 30 October 2017. Retrieved 2017-11-09.
- ↑ Kumar, Vinay; Robbins, Stanley L. (2007). Robbins Basic Pathology (8th ed.). Philadelphia: Elsevier. ISBN 978-1-4160-2973-1. OCLC 69672074.
- ↑ Lawn SD, Zumla AI (July 2011). "Tuberculosis". Lancet. 378 (9785): 57–72. doi:10.1016/S0140-6736(10)62173-3. PMID 21420161. Archived from the original on 27 August 2021. Retrieved 28 July 2020.
